Why vascular access leadership skills are important in the workplace
 I just read a great article on leadership by Stephanie C. from the UK. She states that quality leadership skills are often sought after by many employers; they not only show that you have good interpersonal skills, they also show that you have the ability to co-ordinate, motivate and shape a team. She raises 3 points on what makes leadership skills important in the workplace – points that ring true in our specialty field of practice –
I just read a great article on leadership by Stephanie C. from the UK. She states that quality leadership skills are often sought after by many employers; they not only show that you have good interpersonal skills, they also show that you have the ability to co-ordinate, motivate and shape a team. She raises 3 points on what makes leadership skills important in the workplace – points that ring true in our specialty field of practice –
- Initiative: Often good leadership skills make you more likely to have a good sense of initiative. This means you don’t wait for other’s to tell you to perform tasks or actions. You are forward-thinking and as a result more prepared to deliver solutions to problems that arise.
- Innovativeness: Leadership skills improve your ability to find new ways of doing things in an organisation. You are driven by the ability to change or re-invent common practices, all of which can serve to benefit an organisation.
- Pro-activeness: Leadership skills improve your ability to be proactive. Leaders do not just ‘plan to do’, they actually ‘do’. The ‘do-ers’ are the ones whom are identified as being the most reliable and productive. If you are able to successfully execute written plans into practice, you are showing that you are able to take control of situations rather than just responding to them.
I often hear many vascular access clinicians say they want to change clinical practices within their institutions and facilities. I applaud their desire to make change for the better; for themselves, professionally; for their patients, to provide better care, and for their institution, to improve efficiencies, reduce complications and improve patient safety; however many of them are either frustrated or overwhelmed at the prospect of approaching senior administrators and high level clinicians who may be potential barriers to growth.
It is not with out the 3 elements that Stephanie describes above that change can be implemented. Things that need to be put in place to make these changes are some the following traits that leaders require to help them in their journey to facilitate change.
- Strategic Thinking: Do you think strategically? In this case, what this means is that you often plan effectively for the forthcoming future based on a range of objectives which you set for yourself or your team. Strategic-thinkers are visionary, creative and willing to take risks. They are focussed on the long-term goals and implications of meeting them.
- Decision-making: You can easily choose between one or two courses of action at least 70% of the time. You are able to make firm and prompt decisions with ease despite all of the options available also shows you have exceptional problem-solving skills. A good decision-maker bases their decisions through a good balance of emotional and logical reasoning; this means considering the facts as well as the way in which a decision will effect others.
- Time-management: This skill goes hand in hand with being organised. Do you find it easy to keep to a schedule which you set out for yourself. Are you able to prioritise effectively with tasks and deadlines. This is even more important when you are in the position of leading a team as you will need to effectively map out timelines for others.
- Charismatic: Are you considered to be confident, assertive and/or charming? Leaders possess a certain strength of character and a strong sense of individualism. Charisma is a natural characteristic that makes it easy to influence others. Public speaking skills directly develop your level of charisma and ability to be listened to.
- Listening: Contrary to popular belief, leaders are not always bossy. In fact they are supposed to know when to listen and when to direct. Being able to listen to suggestions and ideas effectively will help a leader implement the correct plans according to their team strengths, weaknesses, concerns and capabilities.
Vascular access specialists have an important role to fulfil within healthcare as others do – however, they also crossover and service nearly all clinical specialties within the healthcare environment as vascular access is the most performed invasive procedure globally. If your a clinician who wants to lead change within your team or facility, develop these elements, grab the evidence, inject it into your passion to improve things, and strive forward, recruiting those who will assist you in the process. It is a tough challenge, but in the end the benefits will be much greater for all.
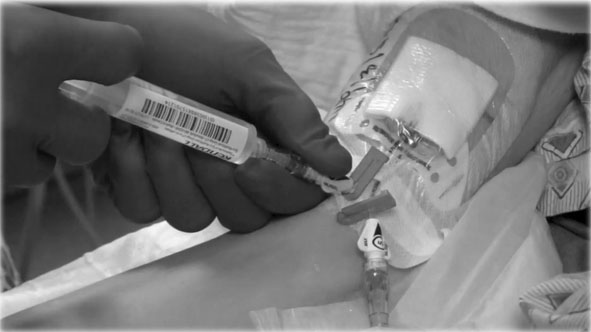
 Air Embolism (AE) is often a life-threatening complication of large bore intravascular device insertion and removal. Although much focus has been with the insertion phase, device removal is just as potentially dangerous.
Air Embolism (AE) is often a life-threatening complication of large bore intravascular device insertion and removal. Although much focus has been with the insertion phase, device removal is just as potentially dangerous.


You must be logged in to post a comment.